
The fact that Black males comprised only 3.1% of medical school enrollment for the 1978-79 school year according to the Association of American Medical Colleges (AAMC) probably isn’t that alarming. After all, it was 1978 – Jimmy Carter was President. Dallas and Grease had just been released, and I was only seven. The shocking and demoralizing realization though is that the comparable stat for the 2019-20 year is actually lower at 2.9% (or nearly unchanged at 3.4% for the “alone or in combination statistic” that includes those identifying with another race as well).
How could it be that over the past forty years with all our “progress” on issues of racial inequity and injustice that that number is actually worse now than then? Indeed, for those who felt the election of a Black president was clear proof that America had moved beyond racism, this single sobering statistic is just one of many to the contrary. NPR analyzed this issue in their 2015 article “There Were Fewer Black Men in Medical School in 2014 Than In 1978.”
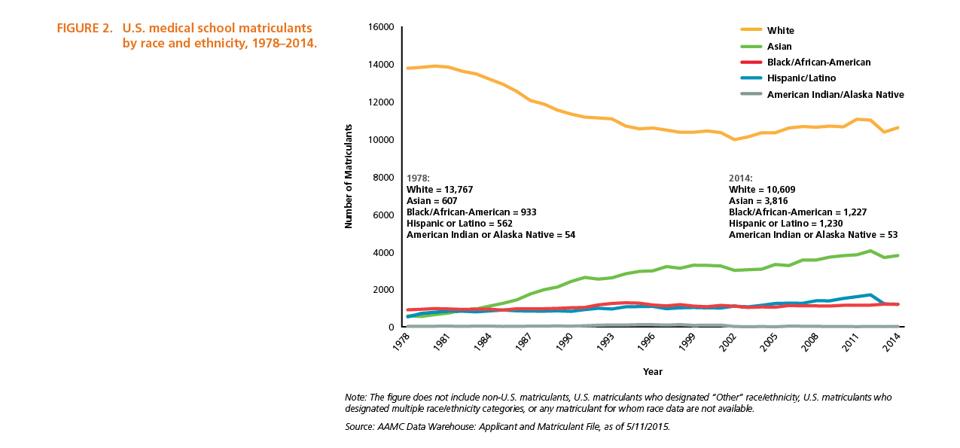
The 2014 AAMC Altering the Course Report indicated that Blacks have typically trailed all other … [+]
AMERICAN ASSOCIATION OF MEDICAL COLLEGES
While the numbers for African Americans are dismal overall, for Black men they’re particularly tragic. Indeed, AAMC’s data shows that the percentage enrollment for African American women actually increased from only 2.2% during the 1978-79 school year to 4.4% during the 2019-20 school year (5.2% when considering those identifying as Black and another race). This begs the question – over the past forty+ years, why haven’t the numbers gotten significantly better for Black men? This is precisely the question tackled in the 2015 AAMC report “Altering the Course: Black Males in Medicine.”
While some may push back on the concept of systemic racism – instead preferring to see inequities as one off aberrations or a result of individual failings – the dearth of Black male doctors in America is arguably a great example of the predictable results of systemic, widespread racism. Arguably, the specific root cause factors are many – all tinged by the reality of racism’s grip on many facets of society including inequities in education, household income, the judicial system, community resources, and many other factors.
Dr. Marc A. Nivet, EVP Institutional Advancement, UT Southwestern Medical Center and primary researcher for the AAMC report insists, “I think the primary problem for Black males in pursuing medicine or any professional career is racism and bias, but it does not take the form we traditionally think of such as closed doors or signs that say Blacks not allowed.” Just recently, the AAMC and the National Medical Association (NMA) the leading voice of African American physicians, announced an action collaborative on Black men in medicine. Their joint statement clearly ties the decades long problem of Black male underrepresentation in medicine to systemic racism. “The root cause is systemic racism dating back to chattel slavery,” explains incoming NMA President Leon McDougle MD, MPH. “This is a societal issue that will require cross-sector investment and collaboration to remedy.”
While no single article can sufficiently analyze the myriad of ways that systemic racism impacts the number of Black men in medicine, let’s explore a range of explicit barriers and challenges that it creates.
Education Disparities
Arguably, the challenges that Black men face pursuing a career in medicine are rooted in the disparities and challenges faced by Black men in life – starting in the classroom.
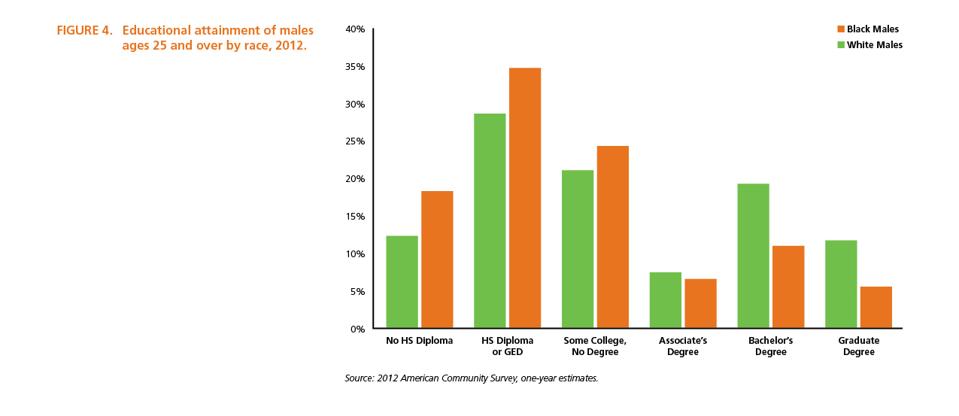
The 2014 AAMC Altering the Course Report reported that Black males significantly trail white males … [+]
AMERICAN ASSOCIATION OF MEDICAL COLLEGES
“America is failing its young Black boys. In metropolitan ghettos, rural villages and midsized townships across the country, schools have become holding tanks for populations of Black boys who have a statistically higher probability of walking the corridors of prison than the halls of college,” concludes the Fall 2011 Educational Testing Service Policy Notes publication. “We fail our Black sons more than any other racial or ethnic group.”
Among the education related barriers/challenges, the AAMC report “Altering the Course: Black Males in Medicine” cites the following disadvantages for Black male youth:
· Higher likelihood of being educated in schools with fewer resources
· Lower levels of participation in gifted or magnet programs
· Lower rates of participation in AP courses
· Lower participation rates in STEM courses
· Higher instances of suspension or disciplinary action (report cites Dr. Ivory Toldson’s research that suggests that contributing factors for this may include lack of cultural awareness among teachers)
While numerous statistics point to a stark achievement gap (arguably fueled by an opportunity gap), Senior Director, AAMC Dr. Norma Poll-Hunter rejects the notion that the students are somehow less able. “It’s not the students that are the problem – not the young Black boys or young men. It’s the system and how the system treats them along the way.” Indeed, Dr. Nivet also cites George W. Bush’s phrase “the soft bigotry of low expectations” as a major factor that starts as early as kindergarten and continues through their academic career. Dr. Poll-Hunter adds “The systemic issues build on each other over time and create a disadvantage that even the best students can’t overcome because the reality is that the system has embedded within it these biases that often determine what talent looks like and where talent should come from.”
Significant Medical School Costs
With medical students carrying an average student loan debt of $200,000 according to the AAMC, medical school simply isn’t feasible for many Black students who are typically coming from significantly less advantaged households. In fact, the Brookings Institute’s analysis of the Black-white wealth gap finds that the net worth of the average Black family is about ten percent that of the average white family. Without strong family support, the reality of medical school is often a mere pipedream for even the best Black students.
Few Black Male Role Models/Weak Support System
The scarcity of Black male doctors also translates into fewer role models for young Black men. “It is hard to be what you don’t see and there are too few minority doctors to begin with, but especially Black male physicians,” explains Dr. Nivet. With fewer Black physicians in the Black community, indeed Black youth often don’t have as strong an extended support network to help socialize them to the pre-med process or just provide moral support and encouragement.
The dearth of Black men in medical school also creates an added pressure once in medical school as they can often feel isolated and internalize added pressure to perform well. “In my medical school class I was one of two Black men,” reflects Olaoluwa Oladipo Fayanju, MD who received a MSc from Harvard University’s T.H. Chan School of Public Health and an MD from Tufts University School of Medicine. “Medical school is a grueling experience without the added pressure of being Black while training.”
Biased Perceptions of Black Men
Black men also face a daunting perception problem. Racism fuels bias and stereotyping that often creates significant barriers that follow them throughout their career. The report concludes, “The most commonly noted challenge is the bias and stereotyping related to the Black male experience in the United States.” Negative perceptions of Black males in the media and throughout society don’t just create bias that impacts teachers, career advisors, admissions counselors and other influencers, but these perceptions can poison how they view themselves and their potential. Unfortunately, for Black males who do succeed in attaining their medical degree despite the odds, these negative perception issues often persist. James E. K. Hildreth, Sr. PhD, MD President and CEO of Meharry Medical College explains “Despite my extensive training and prestigious educational experience, my credibility is often questioned. When we walk into classrooms, boardrooms, operating rooms – we are often first seen by the color of our skin and are only later recognized for our degrees and successes.” Indeed, there are many accounts of patients refusing care from Black doctors. “This puts these physicians in conflicting positions and limits meaningful educational experiences for our nation’s rising generation of medical professionals,” explains Dr. Hildreth.
The Added Social Responsibility
Black medical students and physicians often bear the added burden of working to disprove negative stereotypes and ultimately uplift the entire race. “While my classmates were able to focus on studying, I constantly balanced studying with working to create a pipeline of minority physicians and to maintain an environment of inclusion,” reflects Kevin Stephens, Jr. MD, MBA, Center Medical Director Oak Street Health. Ironically, instead of reveling in their significant professional accomplishments, Black physicians often continue to feel the need to prove themselves. “This ever present need to prove my worthiness that started as an undergraduate continues almost 30 years later as a physician leader,” explains Michele Mitchell, MD, MBA Senior Medical Director, Oak Street Health. “Indeed, my success or failure in a position could be the difference between a door being opened or closed for the next Black physician leader.”

Pritzker School of Medicine students supporting the protests concerning police brutality (2014)
PHOTO CREDIT: ALEX ORTIZ
What’s the Impact?
The lack of diversity in healthcare creates far reaching consequences. Arguably, the most significant negative impact is on health outcomes for Black Americans. “Studies demonstrate that African Americans can have better outcomes when treated by Black doctors,” explains outgoing NMA president Oliver T. Brooks, MD. Among the reasons contributing to this phenomenon is low trust between Black Americans and the American healthcare system. “Many Black Americans have a long-standing history of skepticism in the American healthcare system due to decades of harmful experiments and misuse of medical research including the Tuskegee Syphilis Experiment and the exploitation of Henrietta Lacks’ cells,” explains Dr. Hildreth. “This enduring lack of trust in healthcare impacts preventative care, further contributing to the many health disparities seen today throughout the Black community.” In recent months, as it became clear that people of color have been disproportionately represented in Covid-19 deaths, possibly Black physicians were the least surprised. “The Covid-19 pandemic has highlighted the racial disparities that exist within healthcare,” insists Dr. Mitchell. “Black communities often have fewer resources and less access to healthcare, but there are also fewer physicians in those communities who can truly connect with those patients.” Unfortunately, similar health disparities abound in various areas of medicine.
Perhaps the most tragic consequence of having so few black male physicians is the perpetuation of the cycle. Indeed, the result becomes the cause – and the system continues.
For more info visit: https://www.forbes.com/sites/danabrownlee/2020/08/11/why-are-black-male-doctors-still-so-scarce-in-america/#2f7ad1b027c2
