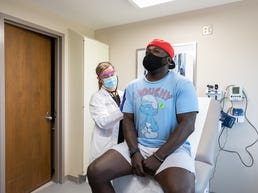
Although the first two large clinical trials of candidate vaccines have managed to include about 3,000 Black participants each, it hasn’t been easy. And later trials might have even more trouble.
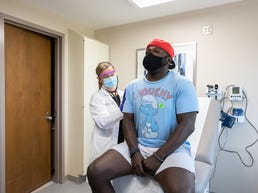
Polls show that among racial and ethnic groups, Black Americans are the most hesitant to get a vaccine once one becomes available, and their skepticism is rising fast. In one September survey, only 32% of Black adults said they would get a vaccine, down from 54% in May.
In a recent focus group run by a foundation that supports the U.S. Food and Drug Administration, Black participants brought up systemic racism for their hesitancy and cited the government-backed Tuskegee Syphilis Study, in which Black men were told they were getting free medical care but instead were denied therapy for their syphilis for decades.
“I firmly believe that this is another Tuskegee Experiment,” one focus group member said.
“We are the ones who are the guinea pigs for the rich,” another said.
“The more they study me, the more they know how to get rid of me,” a third added.
Without adequate Black and Hispanic participation in clinical trials, it won’t be clear whether the vaccine will be safe and effective for them. Although there are no significant genetic distinctions by race or ethnicity, people of color may react differently to a vaccine because of their different lived experiences, experts say.
And if people don’t get vaccinated, they will remain vulnerable to the virus, which has ravaged communities of color in particular. Black Americans are 2½ times more likely to contract COVID-19, nearly five times as likely to be hospitalized with it and twice as likely to die from it, according to the Centers for Disease Control and Prevention.
A vaccine, which is likely to be ready early next year, is considered the best hope for ending the pandemic, but if not enough Americans will get it, then months of effort and $10 billion in taxpayer funding will have been wasted.
To prevent that from happening, the government needs to make a concerted outreach effort to address the concerns of people of color, said Dr. Michelle Williams, dean of the Harvard T.H. Chan School of Public Health in an interview with Dr. Howard Bauchner, editor-in-chief of JAMA, the Journal of the American Medical Association.
“We have to really get to a place where we can reckon with past wrongs and we effectively communicate to this community,” she said. “It means investing in holding intimate conversations around where we’ve done gone wrong and why we have to move past Tuskegee, and think seriously about how African Americans engage in participating in clinical trials.”
Alexandre White, a historian of medicine at the Johns Hopkins School of Medicine, said mistrust needs to be addressed urgently. “We’re seeing a deeply uncoordinated strategy. We’re not seeing a nationally coordinated strategy,” he said.
History of racism remains fresh
America has a terrible history of medical experimentation on Black Americans, including but not limited to Tuskegee, White said.
“The legacies of experimentation and racism date back to the origins of this country and are still quite fresh,” he said.
The country’s first medical colleges purchased enslaved men to dig up freshly buried bodies from Black cemeteries to use for experiments and autopsies, he said.
Dr. James Marion Sims, often considered the “father of American gynecology,” used enslaved women as patients to test new gynecological methods without providing them any anesthesia.
And risk of tuberculosis and other infectious diseases was used historically to justify segregation, White said, as well as “increased medical surveillance, often accompanied by violence, and unsolicited medical intervention.”
Black Americans often learn this history at an early age, he added, while white people aren’t usually taught about it at all.
“At his moment, we’re seeing the horrors of the past and even more recent experiences come home to roost,” White said.
HBCU presidents stick out their arms
When a fellow college president approached Walter Kimbrough and suggested they both join a COVID-19 vaccine trial and then write their communities a letter about it, Kimbrough agreed, much as he doesn’t like needles.
Kimbrough, president of Dillard University, and C. Reynold Verret, president of Xavier University of Louisiana, both historically Black schools in New Orleans, got vaccinated late in the summer. In early September, they wrote a letter to students, faculty, staff, alumni and the broader community.
Kimbrough characterized the letter as saying: “I’m doing it. It’s something you should think about, because there’s a need.”
But the letter took on a life of its own. Although only two students had asked him about it, people on social media – most without reading the letter – accused Kimbrough of all sorts of things, including requiring his students to get vaccinated and taking kickbacks from drug companies for promoting vaccines. Nope and nope.
“Those comments were ridiculous,” he said. If he were really doing those things, people should be trying to get him fired or arrested, not complaining on social media, he added.
Black people aren’t doing themselves any favors by not participating in clinical trials for vaccines and treatments, Kimbrough said. Many likely will get vaccinated eventually anyway – to be allowed back to school or to work. If the vaccine hasn’t been tested on Black people, then it really will be an experiment every time they get a shot, he said.
People willingly put themselves at risk all the time, he added, so why not take a small risk by joining a clinical trial that will benefit others?
“I look at the food that a lot of people eat, the poison that people willingly put in their bodies every day, so how can you tell me you’re mad at me for volunteering to be part of a study that will help you?” he asked. “If you go eat that spicy Popeye’s that’s not helping me, and you’re definitely not helping you.”
Moderna works for trial diversity
Moderna, one of the companies developing a leading COVID-19 vaccine, slowed its clinical trial in September to boost the number of minority participants.
“This was sustained and difficult work,” company president Stephen Hoge said in a phone interview last week. “This was not something I’m aware of anyone doing before.”
The company tried a number of approaches, beginning shortly after the trial launched at the end of July, but the effort really took off this fall, he said. “The last five-six weeks have been a daily grind to build the study we think we needed to provide for confidence.”
Now fully enrolled, the study includes 3,000 Black participants, 10% of the total, and about twice that many Hispanic volunteers. With about 36% enrollees of color, Hoge said the study represents the diversity of the United States.
“People should have confidence in those communities that if the vaccine works in that sample, that they will derive benefit from it as well,” Hoge said.
He credited the study investigators, who built enough trust in the community to spur participation, and the participants themselves, who accepted a personal risk to help others. “That’s always the most inspiring part of this,” Hoge said.
Vaccine hesitancy must be addressed soon
The National Medical Association, which represents African American physicians and patients, has established a task force to review the findings of vaccine trials “to help provide a bridge of communications to the Black community,” said Dr. Leon McDougle, the association’s current president. “Once a safe and effective vaccine is approved, we’d like to be in agreement with that.”
McDougle, who said he will get vaccinated himself when the task force signs off, said vaccine developers have generally supported efforts to diversify their trial participants. But they could be doing more to build long-term relationships in communities of color.
“So, it becomes less of ‘Now that there’s a global pandemic and you’ve received your billion-dollar payment from the government, now you’re coming to us and wanting us to play a role in clinical trials.’ There’s an imbalance there,” he said.
He suggested companies support programs that help the Black community, such as one to lower infant mortality, or provide mentorship to public school students interested in science, such as a program at Ohio State University, where McDougle is an assistant dean and chief diversity officer.
The government, McDougle and others said, has failed to do enough to address the mistrust. In May, for example, the CDC said on its website that people in higher risk groups, should be prioritized for testing even if they don’t have symptoms, McDougle said. “Three days later, that recommendation just disappeared from the website,” he said.
It wasn’t always that way.
In 2009 amid the H1N1 flu pandemic, the CDC made a special effort to reach out to theSomali immigrant community, for example, explain the flu vaccine and address concerns about whether getting one would be compatible with their faith. That helped ease fears and encourage vaccination, said White, the Johns Hopkins medical historian.
Clear communication and “collaborative engagement” can help overcome vaccine hesitancy, he said.
“But these steps need to be taken urgently,” White said. “I don’t think it’s too late, but I think we’re running out of time.”
Contact Karen Weintraub at kweintraub@usatoday.com
Health and patient safety coverage at USA TODAY is made possible in part by a grant from the Masimo Foundation for Ethics, Innovation and Competition in Healthcare. The Masimo Foundation does not provide editorial input.
For more on the original article visit: https://www.usatoday.com/story/news/health/2020/10/29/covid-vaccine-black-americans-hesitancy-trials/3744257001/
